- Home
- About Journals
-
Information for Authors/ReviewersEditorial Policies
Publication Fee
Publication Cycle - Process Flowchart
Online Manuscript Submission and Tracking System
Publishing Ethics and Rectitude
Authorship
Author Benefits
Reviewer Guidelines
Guest Editor Guidelines
Peer Review Workflow
Quick Track Option
Copyediting Services
Bentham Open Membership
Bentham Open Advisory Board
Archiving Policies
Fabricating and Stating False Information
Post Publication Discussions and Corrections
Editorial Management
Advertise With Us
Funding Agencies
Rate List
Kudos
General FAQs
Special Fee Waivers and Discounts
- Contact
- Help
- About Us
- Search

The Open Translational Medicine Journal
(Discontinued)
ISSN: 1876-3995 ― Volume 3, 2014
Impact of Betaine on Hepatic Fibrosis and Homocysteine in Nonalcoholic Steatohepatitis - A Prospective, Cohort Study
Sandeep Mukherjee* , 1, 2, Tamara Bernard1, Kusum Kharbanda1, 2, Anthony J. Barak1, 2, Michael F. Sorrell1, 2, Dean J. Tuma1, 2
Abstract
Introduction:
Nonalcoholic steatohepatitis (NASH) is an important cause of cirrhosis and over the past decade has accounted for an increasing proportion of liver transplants in the United States. Unfortunately there is no treatment for NASH except for risk factor modification. The aims of our study were to assess the impact of betaine on liver function tests, homocysteine levels and hepatic fibrosis in a prospective cohort of NASH patients
Materials and Methodology:
Between July 2003 and June 2006, consecutive patients with NASH were screened to determine treatment eligibility. Eligibility criteria included elevated aminotransferases and a liver biopsy within twelve months of study entry satisfying the Brunt criteria for NASH. Patients were treated with betaine anhydrous 10 grams twice a day for one year. Liver function tests, homocysteine levels and liver biopsy were performed prior to and at the end of treatment. Outcomes were calculated using intention to treat analysis.
Results:
35 patients were eligible. 23 patients completed treatment, seven were intolerant and five dropped out and were lost to follow up. Improvement or normalization in aminotransferases occurred in 62.9% of patients (p<0.05) and in homocysteine in 45.7% (p> 0.05). Resolution or improvement in steatosis occurred in 57.1% (p<0.05), improvement or stabilization of inflammation in 60% (p<0.05) and fibrosis in 62.9% (p<0.05).
Conclusion:
Betaine appears to improve hepatic function tests, homocysteine levels and histology in this cohort of NASH patients. Large randomized studies with long-term follow up are required to assess the effect of betaine for this growing epidemic.
Article Information
Identifiers and Pagination:
Year: 2011Volume: 3
First Page: 1
Last Page: 4
Publisher Id: TOTRANSMJ-3-1
DOI: 10.2174/1876399501103010001
Article History:
Received Date: 7/3/2011Revision Received Date: 8/4/2011
Acceptance Date: 13/4/2013
Electronic publication date: 29 /4/2011
Collection year: 2011
open-access license: This is an open access article licensed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted, non-commercial use, distribution and reproduction in any medium, provided the work is properly cited.
* Address correspondence to this author at the Section of Gastroenterology and Hepatology, 983285 Nebraska Medical Center, Omaha, NE 68198-3285, USA; Tel: 402-559-8859; Fax: 402-559-3434; E-mail: smukherj@unmc.edu
| Open Peer Review Details | |||
|---|---|---|---|
| Manuscript submitted on 7-3-2011 |
Original Manuscript | Impact of Betaine on Hepatic Fibrosis and Homocysteine in Nonalcoholic Steatohepatitis - A Prospective, Cohort Study | |
INTRODUCTION
Nonalcoholic steatohepatitis (NASH) is emerging as an important cause of endstage liver disease and is projected to become one of the leading indications for liver transplantation in the United States in the future [1]. Two common risk factors for the development of NASH are obesity and insulin resistance, important components of the metabolic syndrome, which when successfully treated can lead to improvement of liver function tests and hepatic histology [2, 3]. The metabolic syndrome is also associated with hyperhomocystinemia which in turn is a risk factor for cardiovascular disease [4, 5].
Unfortunately, most patients are unable to either lose weight, comply with a diabetic regimen or more commonly are unrecognized as having these risk factors. Although several recent studies on the medical treatment for NASH have been encouraging there is currently no approved therapy for this highly prevalent condition except for early identification and treatment of risk factors [6, 7].
We report our experience with betaine, a naturally occurring choline metabolite, in a prospective cohort of patients with NASH. The primary aim of our study was to assess the impact of betaine on hepatic fibrosis and the secondary aims were to assess its impact on liver function tests and homocysteine levels.
MATERIALS AND METHODOLOGY
Study Population
Between July 2003 and June 2006, consecutive patients with NASH were screened to determine if they were eligible for treatment with betaine anhydrous (Danisco USA Inc, Ardsley, NY, USA). Eligibility criteria were: elevated aspartate (AST) and alanine amino transferases (ALT) of at least 1.5 times the upper limit of normal; no history of alcohol consumption; normal fasting blood glucose; ultrasound, computerized tomography scan or magnetic resonance imaging demonstrating fatty liver disease; Brunt criteria for NASH and a liver biopsy within twelve months of study entry [8]. Exclusion criteria were patients who were less than 19 or greater than 75 years of age; liver disease of another etiology such as alcoholic liver disease, chronic viral hepatitis, auto-immune liver disease, primary biliary cirrhosis, primary sclerosing cholangitis, hemochromatosis, Wilson’s disease, hemochromatosis or hepatocellular carcinoma; diagnosis of diabetes mellitus within three months of study entry with high probability of starting oral hypoglycemic or insulin therapy during study period; co-morbidities expected to limit life expectancy to less than two years; decompensated liver disease characterized by variceal bleeding, encephalopathy or ascites; patients listed for liver transplantation; prior treatment with betaine; currently pregnant or lactating and inability to provide informed consent.
All patients provided written informed consent prior to study entry. This study was approved by the Institutional Review Board at the University of Nebraska Medical Center.
Treatment Protocol
All patients were followed prospectively. Patients were prescribed betaine anhydrous 10 grams twice a day dissolved in orange juice for one year. Weight in kilograms and plasma homocysteine levels were measured at baseline and repeated at end of study. Liver function tests, defined as AST, ALT, alkaline phosphatase and bilirubin, were performed every three months during patient visits and at study completion.
If worsening of liver chemistries were noted, liver function tests would be repeated in two weeks. Pronounced worsening of liver biochemistries, defined as a four fold elevation of aminotransferase, alkaline phosphatase or bilirubin, either singly or in combination, would result in dose reduction of 3 grams of betaine per day. Repeat values would be repeated at two weeks and dose reduction by 3 grams per day continued every two weeks until liver function tests returned to less than a four fold elevation or the patient was receiving a total dose of 6 grams per day. Dose reductions for unexpected gastrointestinal side effects were also performed in an identical manner every two weeks until the patient was asymptomatic or receiving a total of six grams per day. If betaine was not tolerable at 6 grams per day as defined by a more than four fold elevation of liver chemistries or gastrointestinal side effects, betaine was discontinued and the patient withdrawn from the study.
Liver Biopsies
Liver biopsies were performed within twelve months of study entry and repeated at the end of treatment. Biopsies were stained with hematoxylin and eosin and Masson’s trichrome. They were interpreted by a hepatic pathologist unaware of the clinical data and scored according to the Brunt criteria.
Statistical Analysis
Statistical analysis was performed using Stata version 8 (College Station, TX, USA). Comparison between pre- and post-treatment values was tested with the paired t test. A P value of less than 0.05 was considered to be statistically significant. Outcomes were calculated using intention to treat analysis.
RESULTS
There were 35 patients in the study (29 females, six males) with a median age of 44 years. 23 patients completed treatment, seven were intolerant and five dropped out and were lost to follow up. Three patients were diagnosed with non-insulin dependent diabetes mellitus during the study by their primary care physician and started on metformin 500 mg three times a day.
Biochemical Response
Of the 23 patients who completed treatment, ALT improved or normalized in 95.7% of patients (normalized n =20, improved n= 2, worsened n=1 in patient who gained weight during treatment). AST also improved or normalized in 95.7% (normalized n=21, improved n=1, worsened n=1 in the patient who gained weight). Alkaline phosphatase improved or normalized in 91.3% (normalized n=19, improved n=2, worsened n=1 in a patient who gained weight). Bilirubin values were within the normal range pre-and post-treatment in all patients. Serial homocysteine levels were performed in 16 patients of whom improved values were noted in 9 patients (57.3%). In an intention to treat analysis, improvement or normalization in ALT and AST and were noted in 62.9% of patients, alkaline phosphatase in 60% and homocysteine in 45.7%.
Histological Response
Fat content decreased in 87% of patients (fat disappeared n=5, improved n= 15) and was unchanged in 3; grade of inflammation decreased or was unchanged in 91.3% of patients (decreased n= 15, unchanged n= 6 and worsened n= two patients, of whom one gained weight during treatment) and fibrosis decreased or as unchanged in 95.7% of patients (decreased n= 11, unchanged n= 11, worsened n=1). Of the 11 patients who had decreased fibrosis on their post-treatment biopsy, 4 (36.4%) had an improvement in fibrosis of at least two stages. In an intention to treat analysis, resolution or improvement in steatosis occurred in 57.1%, improvement or stabilization of inflammation in 60% and fibrosis in 62.9%.
Side Effects
Treatment was discontinued prematurely in seven patients (20%) within one month of treatment despite dose reduction according to treatment protocol. Indications for treatment discontinuation were bloating (n=2), diarrhea (n=2), halitosis (n=1) and heartburn (n=2).
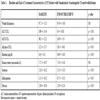
Statistical Analysis.
Statistically significant changes were noted in ALT, AST, Alkaline phosphatase, fat content, grade of inflammation and stage of fibrosis in patients treated with betaine when compared to their pre-treatment values (Table 1).
DISCUSSION
Although advances have been achieved in understanding the pathophysiology and natural history of NASH, this has not been accompanied by a parallel increase in treatment options and no approved therapy currently exists for this common condition. Until recently, most studies have not incorporated serial liver biopsies but used liver function tests as an important end point, a poor surrogate marker for hepatocellular injury in patients with NASH [9]. Despite these concerns, encouraging results have been reported with a variety of medications targeting different points in the pathophysiological spectrum of NASH and include insulin sensitizers, anti-oxidants, agents which interfere with fat absorption and various combinations of these agents [10].
Betaine is a choline derivative whose mechanism of action in fatty liver disease remains to be fully elucidated. Animal studies have demonstrated that it acts as an important methyl-donor for the conversion of homocysteine to methionine and also appears to be the only source of methyl groups for this key metabolic pathway under circumstances of cobalamin or folate deficiency [11]. Betaine can also substitute for S-adenosylmethionine for the direct methylation of phosphatidyl ethanolamine to phophatidylcholine formation, an integral component of very low density lipoproteins. This is the only method by which fat can be exported from hepatocytes, supporting betaine’s unique role as a lipotrope. It remains unclear why a betaine-deficient state may exist in patients with NASH but may be due to the tremendous influx of free fatty acids which overwhelm hepatic stores for phosphatidycholine sysnthesis, leading to fatty infiltration [12].Other effects of betaine include its actions on oxidative stress, transsulfuration reactions and activation of adenosine mono phosphate-activated protein kinase (AMPK) [13, 14].
Our study demonstrates that in patients who tolerated treatment, betaine resulted in marked improvement in hepatic steatosis, grade of inflammation, stage of fibrosis and in hepatic biochemistries, particularly AST and ALT. Interestingly, weight gain, which can worsen hepatic biochemistries and histology in patients with fatty liver disease, was noted during the study period. This increase in weight had no impact on liver chemistries or histology probably either because this change was not statistically significant or betaine counteracted any deterioration of these variables. A further interesting finding was the improvement of homocysteine levels in 57% of patients. As hyperhomocystenemia is a surrogate marker for underlying metabolic syndrome and a risk factor for cardiovascular disease, this finding may be clinically significant as recent studies have also reported that the most important cause of mortality in this patient population is cardiovascular disease [15].
Despite these encouraging findings there were important limitations in this study. Our findings would have been strengthened if we had conducted a randomized study with a placebo arm. Serial homocysteine levels were only obtained in 16 patients further limiting the interpretation of these values in the absence of a control. A recent randomized study comparing betaine with placebo in NASH which has gained widespread attention also showed no evidence of effectiveness on hepatic fibrosis and appears to have relegated betaine’s role for NASH therapy [16]. However, there were several important limitations in this study which merit review and may be pertinent to our study. The most salient was the high drop-out rate in the betaine arm (33% versus 9% for placebo, p <0.05) which meant this randomized controlled study lacked power to detect a statistically significant difference between the two groups. Furthermore it remains unclear what the optimum dose and preparation for betaine are required for NASH. The investigators extrapolated betaine anhydrous doses used in patients with homocystinuria which may have contributed to the study’s negative findings due to the high drop-out rate and loss of power. It is possible a lower dose of betaine anhydrous or a more palatable preparation would have influenced the findings by improving compliance. Betaine levels were also not measure in the urine or plasma [17, 18]. This may have been helpful for confirming patient compliance, particularly in a large study with a drop-out rate which may have been under-estimated. The investigators also reported that a significant proportion of patients had advanced fibrosis (stage 3-4 fibrosis) but descriptive statistics are lacking. This may be clinically relevant as cirrhosis usually takes several years to develop [19]. It would appear extremely unlikely for hepatic fibrosis to significantly improve after only one year of therapy although the authors later reported that betaine may protect against worsening steatosis during this treatment period. Recent studies in animal models of fatty liver disease suggest a re-evaluation of betaine for NASH may be appropriate. Wang et al. reported that betaine supplementation in a high-fat mouse model improved hepatic histology by enhancing adipocyte insulin signaling and correcting abnormal adipokine synthesis [20]. A subsequent study by Kathirvel et al. demonstrated that betaine both prevented and treated mouse models of nonalcoholic fatty liver by improving insulin receptor substrate -1 phosphorylation with resultant improvement in downstream signaling pathways for gluconeogenesis and glycogen synthesis [21].
Despite the lack of a control arm in our study, our findings were encouraging as both hepatic biochemistries and histology improved in a large majority of patients. Although it is possible that sampling issues may have accounted for some of the improvements in fibrosis, we were pleased that 36.4% of patients with improved fibrosis scores were downstaged by at least two stages, a finding most likely attributed to betaine rather than sampling error [22]. Our findings may have also been enhanced if we had prolonged betaine therapy for NASH. However, the optimum duration of treatment remains unclear but may be indefinite in patients without typical risk factors for NASH or do not respond to risk factor modification [23, 24]. Three of our patients were also started on metformin during the study by their primary care physician for new onset diabetes mellitus - all these patients demonstrated an improvement in liver enzymes although hepatic fibrosis was improved, unchanged or worsened in one each. It is possible these findings were confounded by metformin which has been investigated in NASH but not in the presence of diabetes and also acts by enhancing AMPK activation [25]. Betaine intolerance was also an important issue in 20% of patients whose symptoms resolved rapidly after treatment discontinuation. However, aside from mild gastrointestinal side effects, no serious adverse effects were observed with betaine which has been viewed as a safe supplement for a variety of diseases and also associated with a positive impact on quality of life in patients with NASH [26].
CONCLUSION
The findings of our study suggest that betaine may have an important role in the treatment of patients with NASH as there was an improvement in hepatic fibrosis in serial biopsies, despite patients gaining weight during the study period. It is possible multiple medications may be required to achieve histological improvement in NASH. Homocysteine levels also decreased with betaine which may be associated with a reduced incidence of cardio-vascular side effects although this will need confirmation in longitudinal studies. Based on these results, betaine appears to have an important role in the treatment of NASH and its effectiveness needs to be confirmed in large, multicenter randomized studies.
ACKNOWLEDGEMENT
This study was funded by the Clinical Research Center of the University of Nebraska Medical Center, Omaha, Nebraska, USA.