- Home
- About Journals
-
Information for Authors/ReviewersEditorial Policies
Publication Fee
Publication Cycle - Process Flowchart
Online Manuscript Submission and Tracking System
Publishing Ethics and Rectitude
Authorship
Author Benefits
Reviewer Guidelines
Guest Editor Guidelines
Peer Review Workflow
Quick Track Option
Copyediting Services
Bentham Open Membership
Bentham Open Advisory Board
Archiving Policies
Fabricating and Stating False Information
Post Publication Discussions and Corrections
Editorial Management
Advertise With Us
Funding Agencies
Rate List
Kudos
General FAQs
Special Fee Waivers and Discounts
- Contact
- Help
- About Us
- Search

The Open Nutrition Journal
(Discontinued)
ISSN: 1874-2882 ― Volume 15, 2021
Management Strategy of Obesity in the Public Health System: Proposal of a New Model to Optimize Human Resources and Patient’s Motivation
Massimo Pellegrini1, Michael Kob2, Rita Trovato2, Marion Schrei2, Valentina Corazzini2, Nicoletta Facchin2, Mariantonietta Mazzoldi3, Lucio Lucchin2, *
Abstract
Introduction:
Obesity, a disease characterized by an excess of adipose tissue, is a worldwide issue of growing interest in public health.
Methods:
The multifactorial etiology and pathogenesis of obesity strongly orient the scientific community in considering it as a chronic disease without an effective therapy that works for all patients affected by this clinical condition. This leads to a proliferation of non-scientific and dangerous treatment proposals and fake news. The Dietetic and Clinical Nutrition Unit at Bolzano Hospital in Italy has adopted a new strategy based on transparency to optimize time for the first visit and particularly to increase patients’ knowledge and motivation.
Results:
This new strategy provides a preliminary consultation between patients who ask for a nutritional examination and a clinical team composed of a clinician, a dietician and a psychologist. We discuss the preliminary results obtained during the period between February 2010 and March 2016.
Article Information
Identifiers and Pagination:
Year: 2018Volume: 12
First Page: 3
Last Page: 9
Publisher Id: TONUTRJ-12-3
DOI: 10.2174/1874288201812010003
Article History:
Received Date: 17/02/2018Revision Received Date: 15/04/2018
Acceptance Date: 16/04/2018
Electronic publication date: 30/04/2018
Collection year: 2018
open-access license: This is an open access article distributed under the terms of the Creative Commons Attribution 4.0 International Public License (CC-BY 4.0), a copy of which is available at: https://creativecommons.org/licenses/by/4.0/legalcode. This license permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
* Address correspondence to this author at the Dietetic and Clinical Nutrition Unit, Health District of Bolzano, Lorenz-Böhler Street 5, Bolzano, 39100, Italy; Tel: +39 0471 908545; Fax: +39 0471 908707; E-mail: lucio.lucchin@sabes.it
| Open Peer Review Details | |||
|---|---|---|---|
| Manuscript submitted on 17-02-2018 |
Original Manuscript | Management Strategy of Obesity in the Public Health System: Proposal of a New Model to Optimize Human Resources and Patient’s Motivation | |
1. INTRODUCTION
Obesity is a disease characterized by an excess of adipose tissue due to the mutual interaction of several genetic, metabolic, psychological and environmental factors which involves complex neuronal and hormonal patterns. This multifactorial aetiology and pathogenesis strongly orient the scientific community in considering obesity as a chronic disease and not just a risk factor per se [1James WPT. WHO recognition of the global obesity epidemic. Int J Obes 2008; 32(Suppl. 7): S120-6.
[http://dx.doi.org/10.1038/ijo.2008.247] [PMID: 19136980] -7Buffery D. Cardiometabolic risk factors: Novel approaches can improve patient outcomes. Am Health Drug Benefits 2013; 6: 363-4.]. Furthermore, this chronic condition has doubled since 1980 and numbers constantly increase [8Obesity: preventing and managing the global epidemic WHO Technical report series No 894 2000. Available from: http://www.who.int/nutrition/publications/obesity/WHO_TRS_894/en/-26EASO-2015 Milan Declaration: A Call to Action on Obesity A Statement of the members of the European Association for the Study of Obesity to EXPO 2015 2015. Available from: http://gucdv1wwi8pslzdfpv7t0dk6.wpengine.netdna-cdn.com/ wp-content/uploads/2015/06/EASO-Milan-Declaration-FINAL.pdf]. In 2016, the World Health Organization (WHO) estimated that more than 650 million adult people in the world were obese, corresponding to about 13% of the adult population [27WHO | Obesity and overweight [Internet] WHO [cited 2017 Aug 6] Available from: http://www.who.int/mediacentre/factsheets/fs311/en/]. Based on data from Italian National Institute of Statistic (ISTAT) published in 2016, in Italy 5.4 million individuals are obese, corresponding to 10.4% of the adult population [28ISTAT, 2012-2013 Fattori di Rischio per la salute, fumo, obesità, alcool e sedentarietà, anno 2016:tavole 5-10 2016. Available from: https://www.istat.it]. Given the complexity of the pathogenesis of this disease, in which bio-psycho-social factors interact with each other, we still do not have an effective therapy that works for all patients. Moreover, it is difficult to precisely predict obesity evolution considering that: a) obese patients’ expectations in terms of weight loss are often too high and unrealistic (weight loss of more than 20-30% of their initial body weight) partially due to lack of communication between patient and clinician, to the economic interests of the diet industry and to the fake news about nutrition [29Foster GD, Wadden TA, Phelan S, Sarwer DB, Sanderson RS. Obese patients’ perceptions of treatment outcomes and the factors that influence them. Arch Intern Med 2001; 161(17): 2133-9.
[http://dx.doi.org/10.1001/archinte.161.17.2133] [PMID: 11570944] , 30Phelan S, Nallari M, Darroch FE, Wing RR. What do physicians recommend to their overweight and obese patients? J Am Board Fam Med 2009; 22(2): 115-22.
[http://dx.doi.org/10.3122/jabfm.2009.02.080081] [PMID: 19264934] ]; b) the drop-out rate from obesity treatment programs is very high [31Moroshko I, Brennan L, O’Brien P. Predictors of dropout in weight loss interventions: A systematic review of the literature. Obes Rev 2011; 12(11): 912-34.
[http://dx.doi.org/10.1111/j.1467-789X.2011.00915.x] [PMID: 21815990] ], with a mean rate of 30-40% within the first year reported in intervention trials [32Dansinger ML, Gleason JA, Griffith JL, Selker HP, Schaefer EJ. Comparison of the atkins, ornish, weight watchers, and zone diets for weight loss and heart disease risk reduction: A randomized trial. JAMA 2005; 293(1): 43-53.
[http://dx.doi.org/10.1001/jama.293.1.43] [PMID: 15632335] ], and with an attrition rate associated with poorer therapy outcomes [33Mitchell C, Stuart RB. Effect of self-efficacy on dropout from obesity treatment. J Consult Clin Psychol 1984; 52(6): 1100-1.
[http://dx.doi.org/10.1037/0022-006X.52.6.1100] [PMID: 6520280] -35Davis MJ, Addis ME. Predictors of attrition from behavioral medicine treatments. Ann Behav Med 1999; 21(4): 339-49.
[http://dx.doi.org/10.1007/BF02895967] [PMID: 10721442] ]; c) in the Italian Public Health System, the reduction of resources implies cost-effectiveness optimization with an average visit time for an obese patient lasting between 20 and 30 minutes, less frequent check-ups and inadequate time to motivate a lifestyle change [36How to Deliver High-Quality Obesity Counseling in Primary Care Using the 5As Framework | JCOM | Journal of
Clinical Outcomes Management | Turner White Available from: http://www.jcomjournal.com/how-to-deliver-high-quality-obesity-counseling-in-primary-care-using-the-5asframework-2/-38Howe M, Leidel A, Krishnan SM, Weber A, Rubenfire M, Jackson EA. Patient-related diet and exercise counseling: Do providers’ own lifestyle habits matter? Prev Cardiol 2010; 13(4): 180-5.
[http://dx.doi.org/10.1111/j.1751-7141.2010.00079.x] [PMID: 20860642] ]; d) there is a negative stigma associated with obesity that is still too high and that patients should be preliminarily relieved about their condition [39Puhl RM, Heuer CA. Obesity stigma: Important considerations for public health. Am J Public Health 2010; 100(6): 1019-28.
[http://dx.doi.org/10.2105/AJPH.2009.159491] [PMID: 20075322] ].
It is strategic to communicate preliminarily the treatment plan to the obese patient in order to limit the disorientation and the attraction towards the commercial therapeutic illusions and towards unqualified professionals. For this reason, obese patients may experience negative consequences, both psychologically and clinically. Physicians, in primis, and the other health workers who are involved in the treatment of this clinical condition, have the ethical and deontological need to explain their professional background, besides the intervention model that they are willing to adopt [40van Genugten L, van Empelen P, Flink I, Oenema A. Systematic development of a self-regulation weight-management intervention for overweight adults. BMC Public Health 2010; 10(10): 649.
[http://dx.doi.org/10.1186/1471-2458-10-649] [PMID: 20979603] ]. The Italian legal system requires transparency of services as a given criterion, (Ministerial Decree 19th May 1995 Official Journal number 125, “General reference framework of Public Service Charter”). Even though this document is addressed to healthcare companies, it is desirable to disseminate it to the single operative units that deal with chronic pathologies. In order to explain preliminarily the treatment to the obese patient, it is desirable to communicate: 1) entity, organisation chart and qualifications of the operators; 2) way of access into the structure; 3) privacy safeguard; 4) quality standards of the Unit (number of treatments per year, drop-out rate after 6/12/24 months, average weight loss after 6/12/24 months, etc.); 5) therapeutic model used with the relative informed consent [41Lucchin L, Sbraccia P, Nisoli E, Vettor R. Overview of the management of obese patients.Clinical Management of Overweight and Obesity Springer Switzerland EDS 2016; 3-12.
[http://dx.doi.org/10.1007/978-3-319-24532-4_1] ].
Before starting a treatment for obesity, detailed information about the contents of this treatment should be given. This part takes about 10 minutes during the first visit. As this preliminary information is the same for all the obese patients, an initial group meeting with all the subjects who require a visit during the same period may result useful to save time.
Based on the clinical experience of specialists, and also from our experience, the average time should last between 45 and 75 minutes for the first medical examination and between 20 and 30 minutes for subsequent medical checks. It is important to remember to plan how much information has to be given, remembering that each patient memorizes just a little percentage of what doctor says. It has also to be taken into consideration that attention level is at its lowest after 30 minutes of speech and patients tend to forget 40%-60% of medical warnings in a couple of days. Repeating the principal concepts, remembered information grows up to 30% [42Bertakis KD. The communication of information from physician to patient: A method for increasing patient retention and satisfaction. J Fam Pract 1977; 5(2): 217-22.
[PMID: 894226] ]. It is important not to give too much information at one time. Besides, it is important to remember that the patient wants to be more informed about lifestyle modifications and about the prognosis of the disease [43Kindelan K, Kent G. Patients’ preferences for information. J R Coll Gen Pract 1986; 36(291): 461-3.
[PMID: 3440990] ].
With the aim of improving the obesity treatment program and optimizing available time and resources, the Dietetic and Clinical Nutrition Unit at Bolzano Hospital, Italy (International Quality Management System Standard UNI EN ISO 9001 certification by Lloyd's Register since 1995) has devised a new operative strategy to ensure clarity and to provide obese patients with adequate and correct information about the therapeutic plan. The proposed strategy provides a monthly multidisciplinary preliminary group meeting in which a clinician, together with a dietician and a psychologist, illustrate the different treatment phases to groups of patients who have scheduled a nutritional examination in the previous month. For this meeting, patients do not pay a ticket. Before the group meeting, each patient receives the Unit’s Services Booklet (used since 1997 in our Unit and currently at its VII edition) containing transparency’s information and a questionnaire to define the urgency level. These preliminary meetings, addressed to about 250 new patients every year in our experience, aim to achieve a superior therapeutic adherence and a better weight loss maintenance in the long term by showing obese patients the therapeutic pathway they should follow and by encouraging them to approach it.
2. PATIENTS AND METHODS
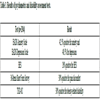
Since February 2010, all obese patients who have required visit/treatment for obesity at our Unit for the first time, have been invited to an obligatory group meeting, which takes place monthly and lasts an average of 75-85 minutes, the first 30 minutes of which are dedicated to the administration of tests for the assessment of obesity and eating disorders-related behaviours and for the assessment of psychosocial variables. The meeting contents are listed in Table 1.
Briefly, during the meeting, a qualified team composed of a physician, a dietitian and a psychologist, illustrates to the participants the physiology of obesity, the techniques to obtain weight loss, the challenges to face in achieving weight reduction and the obstacles to maintain it. Patients are encouraged to focus on their goals of weight reduction and lifestyle change.
The following tests are dispensed during the meeting: a) Hospital Anxiety and Depression (HADS) scale [44Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand 1983; 67(6): 361-70.
[http://dx.doi.org/10.1111/j.1600-0447.1983.tb09716.x] [PMID: 6880820] , 45Snaith RP. The hospital anxiety and depression scale. Health Qual Life Outcomes 2003; 1: 29.
[http://dx.doi.org/10.1186/1477-7525-1-29] [PMID: 12914662] ]: to assess general anxiety and depression; b) 36-Items Short Form Survey (SF-36) [46Questionario sullo stato di salute SF-36 Apolone Giovanni, Mosconi Paola, Ware John Jr Available from: http://guerini.it/index.php/questionario-sullo-stato-di-salute-sf-36.html]: a psychometric questionnaire that allows patients to describe perceived health; c) Binge Eating Scale (BES) [47Gormally J, Black S, Daston S, Rardin D. The assessment of binge eating severity among obese persons. Addict Behav 1982; 7(1): 47-55.
[http://dx.doi.org/10.1016/0306-4603(82)90024-7] [PMID: 7080884] ]: to assess binge eating behavioural disorders; d) SIO-Obesity correlated disability (TSD-OC) test [48Donini LM, Cuzzolaro M, Spera G, et al. Obesity and eating disorders. Indications for the different levels of care. An Italian Expert Consensus Document. Eat Weight Disord 2010; 15(1-2)(Suppl.): 1-31.
[PMID: 20975326] , 49Donini LM, Brunani A, Sirtori A, et al. Assessing disability in morbidly obese individuals: the Italian Society of Obesity test for obesity-related disabilities. Disabil Rehabil 2011; 33(25-26): 2509-18.
[http://dx.doi.org/10.3109/09638288.2011.575529] [PMID: 21542694] ]: for obesity-related disabilities conceived by the “Italian Society of Obesity” (SIO); e) a general Grading Test for the group consultation.
Demographic data, anthropometric measurements, results from psychometric and grading tests and clinical information about therapeutic adherence were retrospectively reviewed. Means and standard deviations were calculated for each item using LibreOffice Calc software version 5.1.2.2.
3. RESULTS
During the period between February 2010 and March 2016, a total of 1501 people have required a dietary intervention for obesity at the Dietetic and Clinical Nutrition Unit of Bolzano Hospital, with an average of 22.7 (SD ± 4.2) requests per month (corresponding to the total number of obese patients who schedule a medical examination in our Center every month).
After the first visit schedule, only 87 people out of 1501, equal to 5.8%, have not attended the preliminary meeting. During the considered period, of the final 1414 meeting participants, only 112, representing 7.9% of the total, have not attended the medical examination.
Demographic and anthropometric characteristics of these patients are listed in Table 2.
The psychometric tests summary results are listed in Table 3. Tests from 110 patients were not assessable, equal to 9.4% of the total.
Preliminary group session are shown in Table 4.
These data clearly show that preliminary meetings have raised a high grade of interest (4.6/5) leading to a higher level of knowledge about weight loss issues.
CONCLUSION
Our strategy clearly suggests that the activation of a group session at the beginning of the obesity treatment is an effective procedure related to the transparency in the cure that brings to a better awareness and a greater motivation experienced by patients. Only a few patients have refused to participate in the meetings and these subjects probably look for a rapid or miracle-working method, showing a poor motivation. On the contrary group meeting, participants manifest to appreciate this not conventional approach to a specialized visit in a Public Service (Table 4).
Thanks to the group session, the time needed for the first individual visit was reduced from an average of 60 minutes to 45-50 minutes (the time needed to explain preliminary information) without compromising the quality of the consultation.
To understand if this strategy has had positive consequences during the course of therapy, we have examined the drop out range before and after the start of the group sessions.
In the period between 2007 and 2009, the mean drop out rate has been 23,3% after 6 months, and 40,6% after 12 months (691 patients). From February 2010 (when the group sessions have started) to March 2016, the mean dropout rate has been 16.40% and 29,80% respectively at 6 months and 12 months. This reduction of about 6% in dropout rate could correspond to those poorly motivated patients who choose not to follow the therapeutic plan.
Moreover, the percentage of those who have had a weight loss of ≥ 4% after 6 months of treatment was 43.6% vs 45,8% for those patients who have started the treatment before 2010. The average weight loss after 6 months was 6,7 ± 5,23 kg (n=1414).
Furthermore, this new approach results in savings resources for the Public Health System due to a higher percentage of patients who are really motivated to undertake the weight loss path, with a decrease in the number of unmotivated overweight and obese people feeding outgoing cases.
We believe that this new therapeutic approach could be useful to increase transparency and show ethics in nutritional treatment to patients as well as it could be useful for clinicians to optimize time in the management of obese patients' first examination.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
No animals/humans were used for studies that are the basis of this review.
CONSENT FOR PUBLICATION
A written informed consent was obtained from all patients when they were enrolled.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGMENTS
The authors would like to thank Mrs. Paola Marchelli for her valuable help in data collection and elaboration and Dr. Giuseppina Pugliano for her precious help in language translation.
REFERENCES
| [1] | James WPT. WHO recognition of the global obesity epidemic. Int J Obes 2008; 32(Suppl. 7): S120-6. [http://dx.doi.org/10.1038/ijo.2008.247] [PMID: 19136980] |
| [2] | Obesity : Preventing and managing the global epidemic : Report of a WHO Consultation on Obesity 1997. Available from: http://www.who.int/iris/handle/10665/63854 |
| [3] | LIGIO Task Force Obesity Italia (TFOI). Linee Guida italiane Obesità Identificare, Valutare, Trattare 1999. |
| [4] | Allison DB, Downey M, Atkinson RL, Billington CJ, Bray GA, Eckel RH, et al. Obesity as a disease: a white paper on evidence and arguments commissioned by the Council of the Obesity Society 2008. [http://dx.doi.org/10.1038/oby.2008.231] |
| [5] | 2012/2013.http://www.sioobesita. org/Standard.pdf |
| [6] | SIO/ADI Standard Italiani per la Cura dell’Obesità 2012/2013 Available from: http://www.sioobesita.org/Standard.pdf |
| [7] | Buffery D. Cardiometabolic risk factors: Novel approaches can improve patient outcomes. Am Health Drug Benefits 2013; 6: 363-4. |
| [8] | Obesity: preventing and managing the global epidemic WHO Technical report series No 894 2000. Available from: http://www.who.int/nutrition/publications/obesity/WHO_TRS_894/en/ |
| [9] | James WPT. The epidemiology of obesity: the size of the problem. J Intern Med 2008; 263(4): 336-52. [http://dx.doi.org/10.1111/j.1365-2796.2008.01922.x] [PMID: 18312311] |
| [10] | Banegas JR, López-García E, Gutiérrez-Fisac JL, Guallar-Castillón P, Rodríguez-Artalejo F. A simple estimate of mortality attributable to excess weight in the European Union. Eur J Clin Nutr 2003; 57(2): 201-8. [http://dx.doi.org/10.1038/sj.ejcn.1601538] [PMID: 12571650] |
| [11] | Branca F, Nikogosian H, Lobstein T, Eds. The challenge of obesity in the WHO European Region and the Strategies for Response: Summary 2007. |
| [12] | Han TS, Tajar A, Lean MEJ. Obesity and weight management in the elderly. Br Med Bull 2011; 97: 169-96. [http://dx.doi.org/10.1093/bmb/ldr002] [PMID: 21325341] |
| [13] | European Commission - Press release - Population projections 2008-2060 From 2015, deaths projected to outnumber births in the EU27 Almost three times as many people aged 80 or more in 2060 2015. Available from: http://europa.eu/rapid/press-release_STAT-08-119_en.htm |
| [14] | Rössner S. Obesity in the elderly-A future matter of concern? Obes Rev 2001; 2(3): 183-8. [http://dx.doi.org/10.1046/j.1467-789x.2001.00034.x] [PMID: 12120103] |
| [15] | Diouf I, Charles MA, Ducimetière P, Basdevant A, Eschwege E, Heude B. Evolution of obesity prevalence in France: An age-period-cohort analysis. Epidemiology 2010; 21(3): 360-5. [http://dx.doi.org/10.1097/EDE.0b013e3181d5bff5] [PMID: 20375843] |
| [16] | Gutiérrez-Fisac JL, Guallar-Castillón P, León-Muñoz LM, Graciani A, Banegas JR, Rodríguez-Artalejo F. Prevalence of general and abdominal obesity in the adult population of Spain, 2008-2010: The ENRICA study. Obes Rev 2012; 13(4): 388-92. [http://dx.doi.org/10.1111/j.1467-789X.2011.00964.x] [PMID: 22151906] |
| [17] | Measuring the Netherlands. A monitoring study of risk factors in the general population, 2009-2010 - RIVM 2010. Available from: http://www.rivm.nl/en/Documents_and_publications/Scientific/Reports/2012/januari/Measuring_the_Netherlands_A_m |
| [18] | von Ruesten A, Steffen A, Floegel A, et al. Trend in obesity prevalence in European adult cohort populations during follow-up since 1996 and their predictions to 2015. PLoS One 6(11): e27455. [http://dx.doi.org/10.1371/journal.pone.0027455] [PMID: 22102897] |
| [19] | Arterburn DE, Crane PK, Sullivan SD. The coming epidemic of obesity in elderly Americans. J Am Geriatr Soc 2004; 52(11): 1907-12. [http://dx.doi.org/10.1111/j.1532-5415.2004.52517.x] [PMID: 15507070] |
| [20] | Li F, Fisher KJ, Harmer P. Prevalence of overweight and obesity in older U.S. adults: Estimates from the 2003 behavioral risk factor surveillance system survey. J Am Geriatr Soc 2005; 53(4): 737-9. [http://dx.doi.org/10.1111/j.1532-5415.2005.53228_10.x] [PMID: 15817035] |
| [21] | Leveille SG, Wee CC, Iezzoni LI. Trends in obesity and arthritis among baby boomers and their predecessors, 1971-2002. Am J Public Health 2005; 95(9): 1607-13. [http://dx.doi.org/10.2105/AJPH.2004.060418] [PMID: 16051931] |
| [22] | Kennedy RL, Chokkalingham K, Srinivasan R. Obesity in the elderly: Who should we be treating, and why, and how? Curr Opin Clin Nutr Metab Care 2004; 7(1): 3-9. [http://dx.doi.org/10.1097/00075197-200401000-00002] [PMID: 15090896] |
| [23] | Zamboni M, Mazzali G, Zoico E, et al. Health consequences of obesity in the elderly: A review of four unresolved questions. Int J Obes 2005; 29(9): 1011-29. [http://dx.doi.org/10.1038/sj.ijo.0803005] [PMID: 15925957] |
| [24] | Villareal DT, Apovian CM, Kushner RF, Klein S. Obesity in older adults: Technical review and position statement of the American Society for Nutrition and NAASO, The Obesity Society. Obes Res 2005; 13(11): 1849-63. [http://dx.doi.org/10.1038/oby.2005.228] [PMID: 16339115] |
| [25] | Villareal DT, Apovian CM, Kushner RF, Klein S. Obesity in older adults: Technical review and position statement of the American Society for Nutrition and NAASO, The Obesity Society. Am J Clin Nutr 2005; 82(5): 923-34. [http://dx.doi.org/10.1093/ajcn/82.5.923] [PMID: 16280421] |
| [26] | EASO-2015 Milan Declaration: A Call to Action on Obesity A Statement of the members of the European Association for the Study of Obesity to EXPO 2015 2015. Available from: http://gucdv1wwi8pslzdfpv7t0dk6.wpengine.netdna-cdn.com/ wp-content/uploads/2015/06/EASO-Milan-Declaration-FINAL.pdf |
| [27] | WHO | Obesity and overweight [Internet] WHO [cited 2017 Aug 6] Available from: http://www.who.int/mediacentre/factsheets/fs311/en/ |
| [28] | ISTAT, 2012-2013 Fattori di Rischio per la salute, fumo, obesità, alcool e sedentarietà, anno 2016:tavole 5-10 2016. Available from: https://www.istat.it |
| [29] | Foster GD, Wadden TA, Phelan S, Sarwer DB, Sanderson RS. Obese patients’ perceptions of treatment outcomes and the factors that influence them. Arch Intern Med 2001; 161(17): 2133-9. [http://dx.doi.org/10.1001/archinte.161.17.2133] [PMID: 11570944] |
| [30] | Phelan S, Nallari M, Darroch FE, Wing RR. What do physicians recommend to their overweight and obese patients? J Am Board Fam Med 2009; 22(2): 115-22. [http://dx.doi.org/10.3122/jabfm.2009.02.080081] [PMID: 19264934] |
| [31] | Moroshko I, Brennan L, O’Brien P. Predictors of dropout in weight loss interventions: A systematic review of the literature. Obes Rev 2011; 12(11): 912-34. [http://dx.doi.org/10.1111/j.1467-789X.2011.00915.x] [PMID: 21815990] |
| [32] | Dansinger ML, Gleason JA, Griffith JL, Selker HP, Schaefer EJ. Comparison of the atkins, ornish, weight watchers, and zone diets for weight loss and heart disease risk reduction: A randomized trial. JAMA 2005; 293(1): 43-53. [http://dx.doi.org/10.1001/jama.293.1.43] [PMID: 15632335] |
| [33] | Mitchell C, Stuart RB. Effect of self-efficacy on dropout from obesity treatment. J Consult Clin Psychol 1984; 52(6): 1100-1. [http://dx.doi.org/10.1037/0022-006X.52.6.1100] [PMID: 6520280] |
| [34] | Wadden TA, Foster GD, Letizia KA, Stunkard AJ. A multicenter evaluation of a proprietary weight reduction program for the treatment of marked obesity. Arch Intern Med 1992; 152(5): 961-6. [http://dx.doi.org/10.1001/archinte.1992.00400170051010] [PMID: 1580722] |
| [35] | Davis MJ, Addis ME. Predictors of attrition from behavioral medicine treatments. Ann Behav Med 1999; 21(4): 339-49. [http://dx.doi.org/10.1007/BF02895967] [PMID: 10721442] |
| [36] | How to Deliver High-Quality Obesity Counseling in Primary Care Using the 5As Framework | JCOM | Journal of Clinical Outcomes Management | Turner White Available from: http://www.jcomjournal.com/how-to-deliver-high-quality-obesity-counseling-in-primary-care-using-the-5asframework-2/ |
| [37] | Pearson WS, Bhat-Schelbert K, Ford ES, Mokdad AH. The impact of obesity on time spent with the provider and number of medications managed during office-based physician visits using a cross-sectional, national health survey. BMC Public Health 2009; 9: 436. [http://dx.doi.org/10.1186/1471-2458-9-436] [PMID: 19948026] |
| [38] | Howe M, Leidel A, Krishnan SM, Weber A, Rubenfire M, Jackson EA. Patient-related diet and exercise counseling: Do providers’ own lifestyle habits matter? Prev Cardiol 2010; 13(4): 180-5. [http://dx.doi.org/10.1111/j.1751-7141.2010.00079.x] [PMID: 20860642] |
| [39] | Puhl RM, Heuer CA. Obesity stigma: Important considerations for public health. Am J Public Health 2010; 100(6): 1019-28. [http://dx.doi.org/10.2105/AJPH.2009.159491] [PMID: 20075322] |
| [40] | van Genugten L, van Empelen P, Flink I, Oenema A. Systematic development of a self-regulation weight-management intervention for overweight adults. BMC Public Health 2010; 10(10): 649. [http://dx.doi.org/10.1186/1471-2458-10-649] [PMID: 20979603] |
| [41] | Lucchin L, Sbraccia P, Nisoli E, Vettor R. Overview of the management of obese patients.Clinical Management of Overweight and Obesity Springer Switzerland EDS 2016; 3-12. [http://dx.doi.org/10.1007/978-3-319-24532-4_1] |
| [42] | Bertakis KD. The communication of information from physician to patient: A method for increasing patient retention and satisfaction. J Fam Pract 1977; 5(2): 217-22. [PMID: 894226] |
| [43] | Kindelan K, Kent G. Patients’ preferences for information. J R Coll Gen Pract 1986; 36(291): 461-3. [PMID: 3440990] |
| [44] | Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand 1983; 67(6): 361-70. [http://dx.doi.org/10.1111/j.1600-0447.1983.tb09716.x] [PMID: 6880820] |
| [45] | Snaith RP. The hospital anxiety and depression scale. Health Qual Life Outcomes 2003; 1: 29. [http://dx.doi.org/10.1186/1477-7525-1-29] [PMID: 12914662] |
| [46] | Questionario sullo stato di salute SF-36 Apolone Giovanni, Mosconi Paola, Ware John Jr Available from: http://guerini.it/index.php/questionario-sullo-stato-di-salute-sf-36.html |
| [47] | Gormally J, Black S, Daston S, Rardin D. The assessment of binge eating severity among obese persons. Addict Behav 1982; 7(1): 47-55. [http://dx.doi.org/10.1016/0306-4603(82)90024-7] [PMID: 7080884] |
| [48] | Donini LM, Cuzzolaro M, Spera G, et al. Obesity and eating disorders. Indications for the different levels of care. An Italian Expert Consensus Document. Eat Weight Disord 2010; 15(1-2)(Suppl.): 1-31. [PMID: 20975326] |
| [49] | Donini LM, Brunani A, Sirtori A, et al. Assessing disability in morbidly obese individuals: the Italian Society of Obesity test for obesity-related disabilities. Disabil Rehabil 2011; 33(25-26): 2509-18. [http://dx.doi.org/10.3109/09638288.2011.575529] [PMID: 21542694] |